Hernie Discale
- Les hernies discales sont une pathologie très fréquente chez les chiens et plus rare chez les chats.
- Elles provoquent une compression du tissu nerveux ayant pour conséquence des douleurs et des troubles locomoteurs pouvant aller jusqu'à la paralysie.
- Leur traitement fait le plus souvent appel à la chirurgie avec de bons résultats dans 90 % des cas opérés.
Introduction
Les hernies discales sont provoquées par l'effraction, dans le canal vertébral, d'une partie du disque intervertébral. Cette intrusion provoque une compression du tissu nerveux.
Les hernies discales peuvent se produire à l'étage cervical, thoraco-lombaire ou lombaire. Elles sont plus fréquentes au niveau thoraco-lombaire.
Les conséquences de la compression médullaire sont : des douleurs et surtout des troubles locomoteurs pouvant aller jusqu'à la paralysie.
Eléments anatomiques
Le disque intervertébral est un "coussin" de fibrocartilage qui unit les vertèbres par leur partie ventrale qui est le corps vertébral.
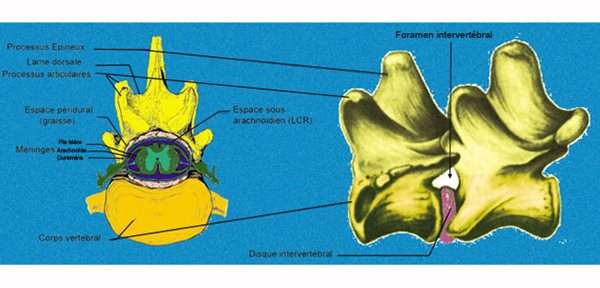
Le disque intervertébral est composé de deux parties : un noyau gélifié (le noyau pulpeux) entouré d'un anneau fibreux dont l'épaisseur dorsale est plus faible que l'épaisseur ventrale.
Le disque intervertébral peut dégénérer de deux façons :
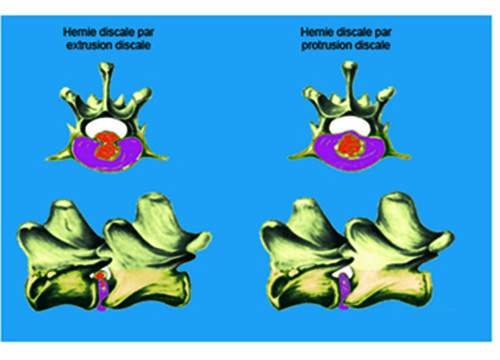
Chez les races dites chondrodystrophiques : Teckel, Pékinois, Cocker, Bouledogue Français, et Beagle entre autres, le noyau pulpeux se transforme en un magma chondroïde plus ou moins calcifié. A la suite d'un mouvement un peu violent ou de mouvements répétés, le disque calcifié passe au travers de l'anneau fibreux dorsal et vient se déverser brutalement dans le canal médullaire en comprimant la moelle épinière : il s'agit d'une hernie discale par extrusion discale. La survenue de la hernie est aigüe et le traumatisme médullaire souvent important du fait de la vitesse d'extrusion du disque. Ce type de hernie discale est dit Hansen I.
Chez les races non chondrodystrophiques : la dégénérescence discale se fait sur un mode fibreux, à la faveur d'une fragilisation de l'anneau discal dorsal, le noyau pulpeux dégénéré fait petit à petit protrusion dans le canal vertébral et vient progressivement comprimer la moelle épinière en entrainant une démyélinisation progressive et une axonopathie irréversible. Cependant, l'évolution de la hernie peut aussi se faire de façon aigüe avec une protrusion plus rapide à la faveur d'un mouvement un peu violent, entrainant une dégradation rapide du statut neurologique avec paralysie brutale. Ce type de hernie appelée Hansen II est plutôt l'apanage des chiens de grand format.
Signes cliniques
Selon l'étage de la compression médullaire, la sémiologie diffère, elle dépend aussi du type de hernie discale présente.
Les compressions médullaires sont classées en cinq stades de gravité croissante :
- Le Stade 1 : qui se manifeste seulement par de la douleur.
- Le Stade 2 : à la douleur s'ajoute une ataxie (l'animal est dit parétique), les signaux nerveux permettant la perception du corps dans l'espace (la proprioception) sont altérés, ainsi que les signaux moteurs, cependant l'animal reste capable de se mouvoir.
- Le Stade 3 : l'animal est paralysé, il conserve par contre le contrôle de ses sphincters urinaires et anaux et perçoit toujours la douleur profonde.
- Le Stade 4 : l'animal est paralysé et ne contrôle plus ses sphincters, il perçoit toujours la douleur profonde.
- Le Stade 5 : l'animal est paralysé, ne contrôle plus ses sphincters et a perdu la sensibilité douloureuse profonde (SDP). La SDP est mise en évidence par pincement des doigts qui doit entraîner une défense de l'animal : il se retourne. Attention, la flexion du membre est un réflexe court et ne signifie pas que l'animal perçoit la douleur.
Selon la position sur le rachis les signes cliniques sont plus ou moins marqués.
Les hernies discales cervicales, du fait de la plus grande largeur du canal médullaire par rapport à la moelle, sont essentiellement douloureuses. L'animal présente une attitude voussée avec une défense marquée à la mobilisation du cou. Plus rarement, des déficits moteurs peuvent être présents, ils commencent toujours sur les membres postérieurs avant, éventuellement, d'atteindre les membres antérieurs. Les cas de paralysie ou de tétraplégie sont rarissimes.
Les hernies discales thoracolombaires peuvent présenter tous les stades cliniques. Les paralysies avec paraplégie sont extrêmement fréquentes. Elles constituent en général une urgence chirurgicale.
Les hernies lombaires basses et lombosacrées sont responsables d'une pathologie nommée syndrome de la queue-de-cheval. A ce niveau là du rachis, il s'agit d'une pathologie de l'étage radiculaire correspondant à la sciatique de l'homme. Les premiers et constants signes cliniques sont une douleur à la palpation et une réticence à se mouvoir. La pathologie peut évoluer sur un mode chronique avec apparition progressive de troubles moteurs et sphinctériens.
Diagnostic
Le diagnostic passe par la réalisation d'examens d'imagerie médicale afin de repérer l'étage et le côté de la hernie.
La myélographie.
C'était l'examen de choix jusqu'à ces dernières années pour le diagnostic des hernies discales, le développement du scanner tend actuellement à le supplanter.
Il s'agit d'un examen radiologique sous anesthésie. Un produit de contraste iodé radio-opaque est injecté dans l'espace sous arachnoïdien. Des clichés sont alors effectués pour mettre en évidence des déviations de la moelle épinière ou des modifications de la prise du liquide de contraste.
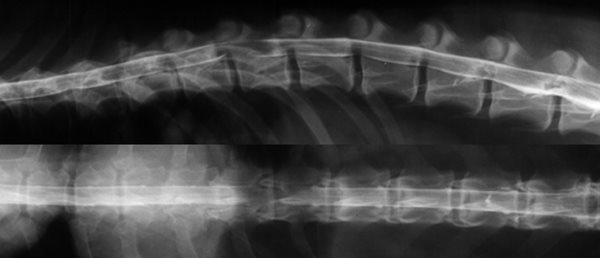
Myélographie Hernie Discale T12-T13
La myélographie est souvent suffisante pour établir un diagnostic et poser l'indication chirurgicale, cependant dans certains cas, en présence d'un gros oedème médullaire ou de difficultés de latéralisation, il peut être nécessaire d'avoir recours à des moyens d'imagerie tridimensionnels comme le scanner ou l'IRM.
Les imprécisions liées au caractère bidimensionnel de l'examen le rend actuellement obsolète face à la tomodensitométrie numérisée. Son usage peut encore se justifier en situation d'urgence neurologique chirurgicale et en l'absence de disponibilité d'un scanner. La myélographie, avec ses carences, demeure un examen utile, tant par sa simplicité de réalisation que par sa grande accessibilité matérielle (un simple appareil de radiologie permet d'y avoir recours).
Le Scanner ou Tomodensitométrie Numérisée.
Depuis quelques années, le développement du scanner en médecine vétérinaire (imagerie par tomodensitométrie numérisée) s'est fortement accéléré avec la multiplication des structures équipées.
Le scanner est actuellement l'examen de choix pour le diagnostic des hernies discales chez les carnivores domestiques et d'une façon générale pour l'exploration des pathologies du rachis. Ses capacités de dessuperposition des structures anatomiques et sa meilleure résolution spatiale lui permettent, avec les machines de dernière génération, de supplanter définitivement les examens radiologiques sous contraste.
Le scanner permet à la fois une meilleure approche de l'étage de la lésion, mais aussi une meilleure latéralisation de celle-ci, ce qui est capital en cas de geste chirurgical. Il permet aussi, en cas de hernies multiples (ce qui est fréquent dans certaines races comme le Bouledogue français) d'avoir une approche lésionnelle permettant, au travers de critères objectifs, de faire un tri entre les hernies pour isoler celle responsable des symptômes nerveux.
L'examen tomodensitométrie du rachis se fait avant et après injection de produit de contraste iodé pour rehausser les lésions. Dans certains cas extrêmes, et au demeurant rarissimes, une injection complémentaire de produit de contraste dans l'espace sous arachnoïdien peut être nécessaire, l'examen réalisé alors se nomme un myéloscanner. Cet examen peut s'avérer très utile, notamment pour le diagnostic de certaines affections rares des méninges nommées kystes arachnoïdiens, présentes en particulier chez le Rottweiler, et dont le diagnostic constitue une des limites du scanner avec le syndrome de Chiari.
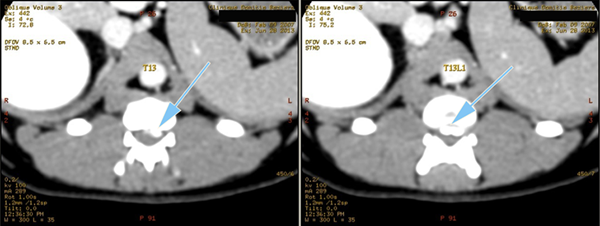
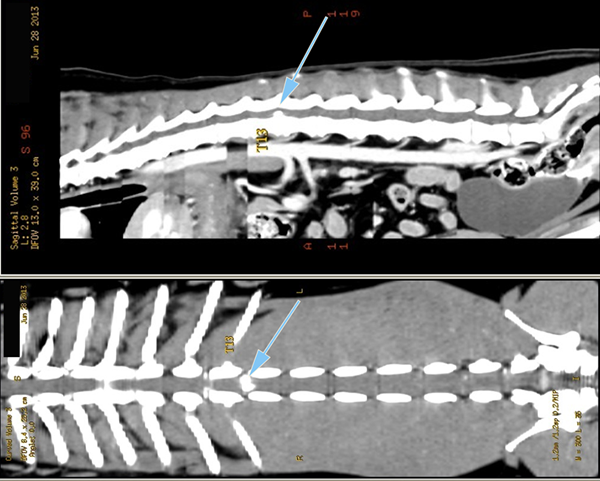
Coupes axiales
Scanner d'une Hernie discale T13L1 extrusive chez un chien reformatages sagittal et coronale
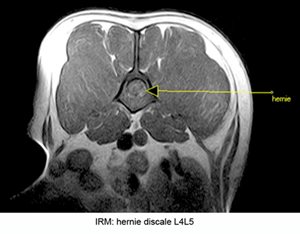
L'imagerie par résonance magnétique nucléaire (IRM).
Si quelques centres vétérinaires sont équipés en appareils dits de "bas champs", le développement de l'IRM en médecine vétérinaire en France reste encore à ses balbutiements. Lla carence en appareils performants dits de "haut champs" est une limite importante quant à la qualité des examens permise par la plupart des appareils actuellement accessibles.
Sur le rachis, sauf pour le diagnostic des kyste arachnoïdiens, du syndrome de Harnold Chiari, ou de certaines lésions intra-médullaires, les machines de bas champs sont moins performantes que les scanners multicoupes (dits multibarettes) désormais facilement disponibles en médecine vétérinaire.
La durée de l'examen par IRM, la très faible répartition géographique des appareils, leur manque de puissance et le coût très supérieur de l'examen par rapport à un scanner, font de l'IRM un examen de deuxième intention en terme d'exploration du rachis en médecine vétérinaire.
Il est par ailleurs important de noter qu'en médecine humaine, où les machines de haut champs très performantes sont pourtant facilement accessible, c'est les scanner qui demeure l'examen de première intention sur la colonne vertébrale.
Traitement Chirurgical
Dans les cas les moins graves et en l'absence de déficits neurologiques, un traitement médical faisant appel aux anti-inflammatoires peut être mis en place. S'il existe des déficits neurologiques moteurs ou sensitifs, ou en l'absence de résultat du traitement médical pour les hernies de stade 1 uniquement algiques, le traitement chirurgical devient impératif.
Selon l'étage de la hernie, la technique chirurgicale diffère. Les hernies cervicales sont généralement traitées par corpectomie, les hernies thoracolombaire par hémilaminectomie ou laminectomie et les hernies de la région lombosacrée par laminectomie dorsale. Le principe de ces interventions est à la fois de permettre une décompression du tissu nerveux et le retrait du matériel discal hernié.
La corpectomie.
Après anesthésie générale, l'animal est disposé en décubitus dorsal.
Le principe est d'aborder le canal vertébral par voie ventrale, en faisant une tranchée au travers des corps vertébraux adjacents pour pouvoir retirer le matériel discal hernié.
L'os est fraisé au moyen d'une fraise neurochirurgicale à très haute vitesse jusqu'au ligament longitudinal dorsal. Le matériel discal peut alors être retiré.
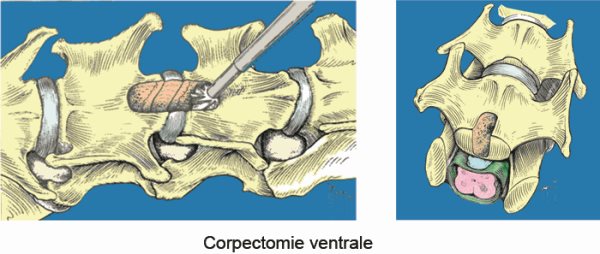
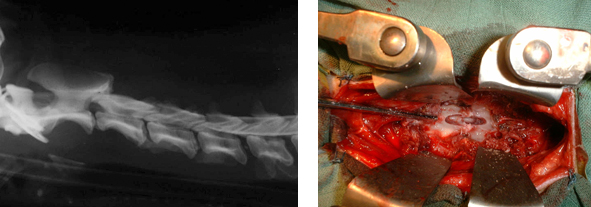
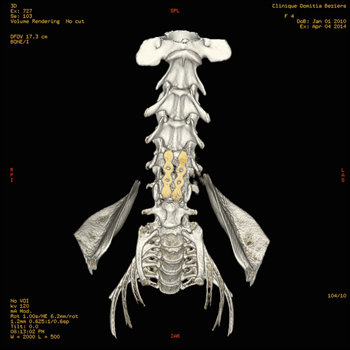
La fenêtre pratiquée dans les corps vertébraux ne doit jamais dépasser la moitié de la longueur et le tiers de la largeur du corps vertébral, au risque d'avoir une luxation du rachis avec télescopage des vertèbres. Chez les animaux de très petite taille, il n'est parfois pas possible de réaliser une corpectomie respectant ces contraintes ; il est alors nécessaire de pratiquer une stabilisation du rachis. Cette stabilisation est réalisée soit au moyen de vis et de ciment chirurgical, soit au moyen de vis et plaques verrouillées en titane.
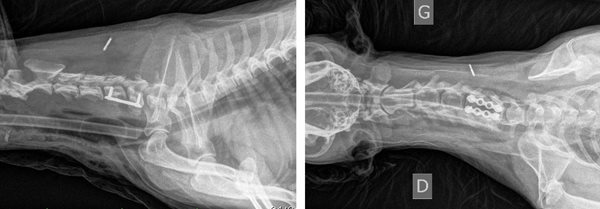
Stabilisation du rachis cervical par vis verrouillées et plaques intersomatiques en titane.
Après corpectomie, la récupération est normalement très rapide. L'intervention est cependant délicate : des risques de saignements abondants sont possibles en cas de lésions vasculaires.
Laminectomie et Hémilaminectomie.
Après anesthésie générale, l'animal est disposé en décubitus ventral.
Le principe est d'aborder le rachis par voie dorsale ou dorsolatérale. Une partie (hémilaminectomie) ou la totalité (laminectomie) de la lame dorsale de la vertèbre est retirée au moyen d'une fraise neurochirurgicale et de rongeurs spéciaux. Il est ainsi pratiqué une fenêtre dans la vertèbre qui permet, à la fois de décomprimer le tissu nerveux, et d'accéder au matériel discal hernié qui peut être retiré.
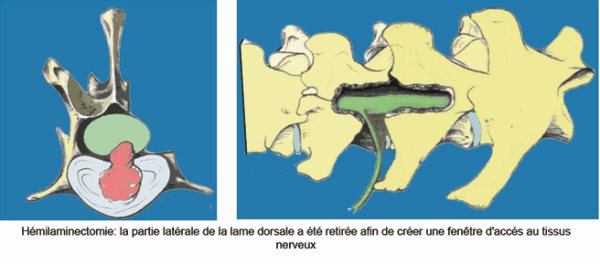
Après laminectomie, les temps de récupération sont variables. Ils dépendent du stade initial des lésions. Plus le stade de la lésion est élevé, plus les temps de récupération sont longs, ils varient de quelques jours à plusieurs mois. Ils dépendent aussi de l'étage de la hernie discale, les hernies lombaires basses en territoire radiculaire récupèrent beaucoup plus vite que les hernies de l'étage thoracolombaire.
Pronostics
L'élément clef du pronostic est le stade initial neurologique.
Les hernies discales de Stade 1 à 3 ont des taux de récupération supérieurs à 90 % avec le traitement chirurgical.
Les hernies discales de stade 4 ont des taux de récupération, selon les hauteurs, entre 85 % et 90 %.
Les hernies de stade 5 sont beaucoup plus difficiles à traiter. Chez les individus opérés immédiatement après la survenue de la paralysie et la perte de sensibilité douloureuse profonde (moins de six heures), on peut espérer des taux de récupération autour de 70 %. Pour les animaux évoluant depuis plus de six heures, les résultats ne font pas consensus. Il est globalement admis qu'entre 6 et 12 heures, 50 % de bons résultats peuvent être attendues et que les taux descendent en dessous de 30 % au-delà de 12 heures (ou 24 heures suivant les hauteurs).
Complications éventuelles
- Indépendamment de la technique, le risque d’accident à l’anesthésie, aussi faible soit il, reste non nul.
- Les infections du site chirurgical sont rares et généralement bénignes.
- Une collection séreuse peut se constituer sur le site chirurgical sans conséquence fonctionnelle.
- Il existe souvent une aggravation du statut neurologique du patient après l'intervention. Cette aggravation est normalement transitoire.
- Malgré le traitement chirurgical et avec des stades neurologiques initiaux corrects, certains patients ne récupèrent pas la motricité. Les hernies de type protrusion discale chronique haute sont celles pour lesquelles l'intervention est la plus délicate.